DOWN LOAD at
Showing posts with label Waveforms. Show all posts
Showing posts with label Waveforms. Show all posts
Friday, July 8, 2016
Thursday, June 16, 2016
Tuesday, September 23, 2014
Flow Patterns and Flow Rates
One corrective action in correcting flow mismatch is switching from a constant flow pattern to a decelerating flow pattern this provides a high initial peak flow. The above video overviews how different flow patterns effect inspiratory flow rates.
RELATED POST/LINKS
Correcting flow mismatch by increasing ventilator flow rate
Creating Flow Mismatch with a Simulator
Oxylog 3000 Simulator
Why I do not use Draeger ventilator simulators
Flow mismatch: patient ventilator asynchrony associated with volume ventilation
Waveform of the week: Flow Mis-match
Decreasing Dyspnea During Mechanical Ventilation
Labels:
Waveforms
Saturday, September 20, 2014
Correcting flow mismatch by increasing ventilator flow rate
Flow mismatch is a common patient ventilatory asynchrony associated with volume ventilation, which may lead to cardiovascular instability, increased oxygen consumption, increased carbon dioxide production, increased patient discomfort and prolonged mechanical ventilation[iv]. Fortunately, flow mismatch can be simply identified with the proper assessment of the pressure waveform.
To correct flow mismatch titrate the flow rate to match the patient’s inspiratory demands. Another corrective action is switching from a constant flow pattern to a decelerating flow pattern this provides a high initial peak flow. One must consider that changes in ventilatory demand may result in unnecessary higher than average assist resulting in ventilator induced diaphragm dysfunction[ii], a lower PaCO2 set-point, and delay in liberation.
RELATED POST/LINKS
Creating Flow Mismatch with a Simulator
Oxylog 3000 Simulator
Why I do not use Draeger ventilator simulators
Flow mismatch: patient ventilator asynchrony associated with volume ventilation
Waveform of the week: Flow Mis-match
Decreasing Dyspnea During Mechanical Ventilation
Labels:
Waveforms
Friday, September 12, 2014
Creating Flow Mismatch with a simulator
I know in the past I stated I did not use Draeger simulators. However this Oxylog simulator is responsive and I will be using it in a few videos. This video demonstrates that with this simulator, one can create "Flow Mismatch" a patient-ventilator asynchrony common in VC-CMV.
RELATED POST/LINKS
Oxylog 3000 Simulator
Why I do not use Draeger ventilator simulators
Flow mismatch: patient ventilator asynchrony associated with volume ventilation
Waveform of the week: Flow Mis-match
Decreasing Dyspnea During Mechanical Ventilation
Labels:
Waveforms
Monday, February 3, 2014
A Synopsis of Strategies in Difficult Intra-Operative Ventilation
 |
| Image from: http://www.esicm.org |
“Strategies in Difficult Intra-Operative Ventilation” was a
continuing education course originally presented at the 2012 American Academy
of Anesthesiologist convention.
Now the
course is available online through the ASA website for continuing education units. I would not recommend this course for the ICU practitioner because it overviews strategies that we practice daily or weekly, however for the anesthesia provider that is not familiar with lung protective strategies the course may be beneficial.
Below is a synopsis of the course and a hyperlink to the website.
Tuesday, November 5, 2013
Whats in your pockets? Are you a Prepper or Macgyver?
In a previous post (The RT Hoarder) I mention that I carry very little on me when I'm at work.
Yes, I believe in being prepared, however I try to practice the "Macgyver" philosophy [1], versus the "Dooms Day Prepper" mentality [2].
This post presents my Everyday Carry (EDC) [3] from when I first started in the field of respiratory therapy to what I carry now. I will describe "what is in my pockets" and why, also notice the progression throughout the years.
What items do I get rid of & what do I always need to practice the profession?
 |
| EDC as a RT student & new graduate. |
Monday, August 12, 2013
Waveform of the Week
Waveform of the week
I posted a patient ventilator asynchrony case on the GMEP Media Gallery.
Here is the link for viewing:
Wednesday, May 8, 2013
Os Gráficos do Ventilador
Os Gráficos do Ventilador
Identificando
a Assincronia Paciente-Ventilador e Otimizando as Definições
AMAZON KINDLE
Labels:
Waveforms
Thursday, September 13, 2012
Dead Falls, Trip Wires, and Ventilator Settings
As many may
not know I grew up in the Midwest and was raised on the principles of self-reliance
and the respect for nature. I was taught how to hunt, fish, trap, forge,
and grow one’s own vegetables. Our family even attempted to save enough food
for a year, preparation for hard times or a catastrophic event (most likely a
tornado).
Labels:
Waveforms
Sunday, August 26, 2012
Volume-Control to Pressure Control
 |
| Image 1: The Settings of VC-CMV. The settings highlighted in yellow are associated with patient-ventilator asynchrony. |
VC-CMV is likely the most utilized mode of mechanical ventilation. This is due to a few a reasons:
1. VC-CMV is a standard mode on almost every intensive care ventilator (table 1).
2. VC-CMV is one of the first modes of mechanical ventilation.
3. VC-CMV is easy to understand in both theory and operation.
4. VC-CMV is the standard of care when ventilating patients with Acute Respiratory Distress
Syndrome (ARDS) and Acute Lung Injury (ALI).
Labels:
Waveforms
Wednesday, July 18, 2012
Vent Graphics Contest WINNERS
First, I would like to thank all my readers who entered the "Vent Graphics Contest" , I appreciate all of the efforts.
First Prize
John Priest
Equipment Used: Epiphan
 |
| Image 1 & 2: Preventing auto-triggering. |
Labels:
Waveforms
Thursday, June 14, 2012
Capture the Flag: Vent Graphics Contest
http://www.youtube.com/user/devinsupertramp
I have many people ask how I create and capture videos of ventilator waveforms. In this post I will describe my techniques and introduce a ventilator screen capture contest for my new book Ventilator Graphics: Identifying Patient Ventilator Asynchrony & Optimizing Settings (2nd Ed).
Here are the contest prizes:
- iTunes gift card ($50), free copy of the new book ($9.99), your screen shot will be used in the new book.
- iTunes gift card ($25) free copy of the new book ($9.99), your screen shot will be used in the new book.
- iTunes gift card ($10) free copy of the new book ($9.99), your screen shot will be used in the new book.
Labels:
Waveforms
Saturday, May 12, 2012
The Importance of Identifying Patient Ventilator Asynchrony
One factor associated with PMV is inappropriate ventilator settings. The below abstract reinforces how ventilator asynchrony increases the likelihood of PMV.
Tuesday, March 27, 2012
Quantifying Patient Ventilator Asynchrony
 |
SERVO-i Ventilator screen. Using NAVA monitoring & captured screen shots to quantify patient ventilator asynchrony.
|
Patient ventilator asynchrony is present in the majority of ventilated patients [1].
One of the most difficult components of patient ventilator assessment is actually recognizing asynchrony. Authors of the following study “Efficacy of ventilator waveforms observation in detecting patient–ventilator asynchrony” ‘[2] demonstrate how challenging identifying asynchrony is, even for the seasoned physician.
Monday, February 6, 2012
"It's a Nail"
 |
“Spoils of War” by Andy Ihnatko 2009.
A colleague of mine described a presentation she attended today in which the speaker was describing the usefulness of the “Dynamic Lung” and how there was no use for those squiggly little lines (referring to ventilators waveforms).
Is this guy serious? |
Labels:
Waveforms
Thursday, September 29, 2011
Waveform of the Week: “Golden Moment”
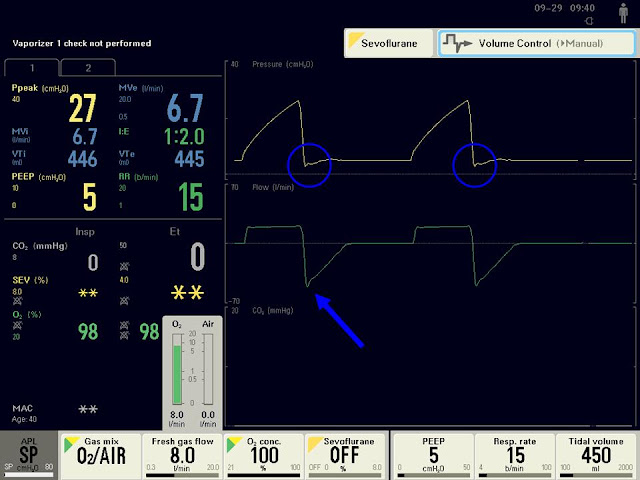 | |||||||||||||||
| Image 1: Screen of the FLOWi anesthesia delivery system, showing the "Golden Moment" highlighted with blue circle. |
It has been over a year since writing a waveform of the week post; however I have incorporated ventilator waveform pictures in recent posts. The waveform for this week is termed the “Golden Moment”
Labels:
Waveforms
Monday, September 19, 2011
Decreasing Dyspnea during Mechanical Ventilation
 | |||||||
| Flow Mismatch Associated with VC-CMV |
Utilizing Volume Control-Continuous Mandatory Ventilation (VC-CMV) may lead to patient ventilator asynchrony [1] and dyspnea. The main reason for these issues is the fixed (constant) flow rate associated with VC-CMV.
Labels:
Waveforms
Friday, June 10, 2011
Sunday, May 15, 2011
The Intrinsic Diaphragmatic Frequency
 |
Image 1: Missed trigger attempts, notice the flow distortions (purple flow waveform) without associated breaths. Ventilator measured rate 12 bpm, however true intrinsic rate 30 bpm.
|
Many patients receiving mechanical have high intrinsic diaphragmatic rates (≥30 breaths per minute) even when very well assisted [1]. This is usually unnoticed because the ventilator only measures machine or patient triggered breaths; however the patient’s true respiratory rate may be higher. This can be problematic when performing a spontaneous breathing trial (SBT) for a couple of reasons.
Labels:
Waveforms
Subscribe to:
Posts (Atom)





